In this section
In This Section
Learning Outcomes
Scenario Environment
Location |
|
Props/Equipment | Chairs, screen to sub-divide large venues |
Make-Up/Moulage | None |
Multi-Media | None |
Personnel | Standardized patient |
Potential Distracters | N/A |
Other | Facilitator |
Scenario Progression
(Case Introduction and Available Collateral Information)
Students work in pairs.
Each student will run through a scenario with a standardised patient.
As one student assumes the role of a radiography student on placement, the other observes and gives feedback after the event.
The standardized patient will also give feedback on how they found the conversation.
Ground rules are established and include:
- Confidentiality – what happens in the room stays in the room. The standardized patient will also keep conversations confidential.
- Feedback must be constructive and supportive.
- Any other appropriate ground rules as agreed by participants.
Instructions for Standardized Patient
Standardized patients are encouraged to visit the MacMillan Cancer support web pages to gain a broad understanding of what radiotherapy is before participating in this activity. The following link can be used:
The following scenario is given to the standardized patient:
You are a patient who is about to have their first external beam radiotherapy treatment for a pelvic cancer e.g. prostate (male) /cervix cancer (female). Typically, this treatment will be delivered daily over a period of days/weeks. Each day you will be expected to lie on the radiotherapy treatment couch in the same position as you would have been in for your radiotherapy planning scan. You may be asked to follow a bladder filling and/or rectum emptying protocol prior to treatment each day.
The student should call you from the waiting area and should introduce themselves to you. They are then expected to perform a 3-point identity check which includes asking your name, date of birth, home address or other identifying data. They may also ask you the site you are expecting to have treated. They should then take you to a private area to explain some of the technical information that you should know before treatment begins. This would typically include:
- An explanation of the treatment process. They should tell you that you will be lying on the treatment couch in the same position as your planning CT scan with appropriate immobilisation equipment in place. You could at this point tell the student that you cannot remember this position and ask them to describe it for you.
- The room lights will be dimmed so that the radiographers can see the room lasers and the radiation field lights to make sure that you are in the correct position for your treatment. You could ask the student to explain what would happen if you were not in the correct position.
- The student should explain that the radiographers will move the treatment couch and will also move you into the correct position for treatment. They should encourage you not to try to help the staff. They will move you!
- Sometimes some images (x-rays) may need to be taken to confirm that you are in the right place. At this point you may wish to ask the student if the radiographers can see on the images if your cancer has spread.
- You should also be told that the treatment machine (or linac) may move around you but that it will not touch you.
- You should be told to lie as still as possible and that the radiographers will leave the room when they are ready to deliver the treatment. They may explain that an alarm will sound as they leave the room.
- You should be told that the radiographers can see you at all times on CCTV and that if you need anything you can raise your hand.
- The student may also tell you that the machine will make a noise when delivering the treatment but that you will not feel anything.
You can ask any questions that you think you would like more information on at any point in the conversation. Possible questions could include:
- Will I be radioactive after my treatment?
- What will happen if I cannot come for one of my radiotherapy appointments?
- Can my husband/wife/partner stay in the treatment room with me?
- Can I drive after my treatment?
- Will I feel sick after my treatment?
The student should then tell you about possible side effects of your treatment and the management of the side effects should they occur. The following links may give you some idea about the information that the students should discuss with you:
Skin care advice for radiotherapy patients
You can also add more to your character – e.g. you may be anxious because you think these side effects mean your cancer is spreading, you could be stressed/angry because you could not park or you need to get into work.
We want the students to appreciate, even as a first-year student, patients will ask them questions. They will not know all the answers and we would not expect them to, but they should know what to say about finding out information for them, rather than make something up. Students usually build up a rapport with patients because they are seeing them daily and collect them from the waiting room for the radiographers.
Students may ask you more about the symptoms you are experiencing (how long have you been experiencing them, your diet, how much you are drinking) and/or they may reassure you these are usual treatment side effects (which they are!).
The student should then give you an opportunity to ask any questions that you may have. They could also signpost you to useful resources/ websites.
The student should the confirm that you consent to your first treatment. This would then bring the session to an end.
Evaluation Strategy
The following observation checklist may be used as a guide:
First day chat observation checklist.xlsx
Debrief after Simulated Activity
The facilitator will then host a debrief session with the students which could also include input from the standardized patient. A structured debrief is recommended and could include the utilization of the debrief diamond (Jaye et al., 2015).
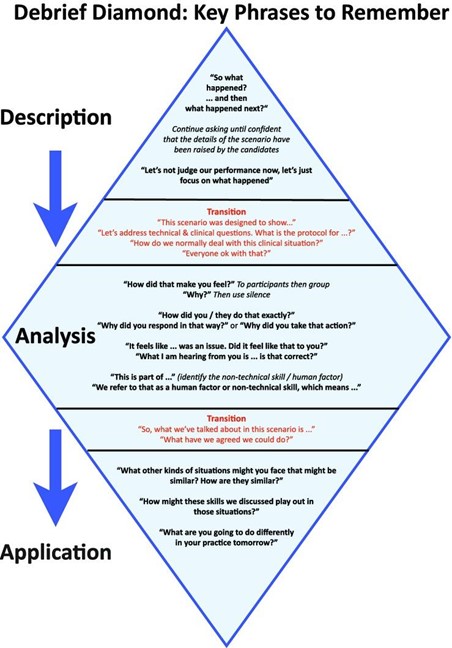
Link to Evidence Base
Skin care advice for radiotherapy patients
Jaye, P., Thomas, L. & Reedy, G. (2015). The Diamond: a structure for simulation debrief. The clinical teacher 2015; 12: 171–175